The Measles Mystery
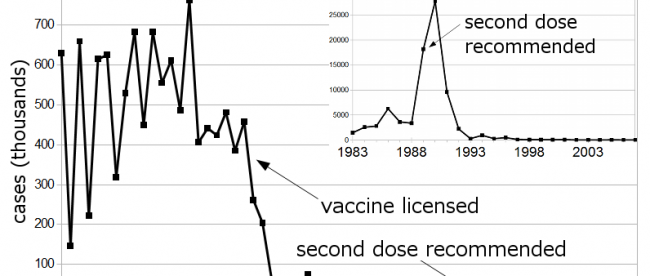
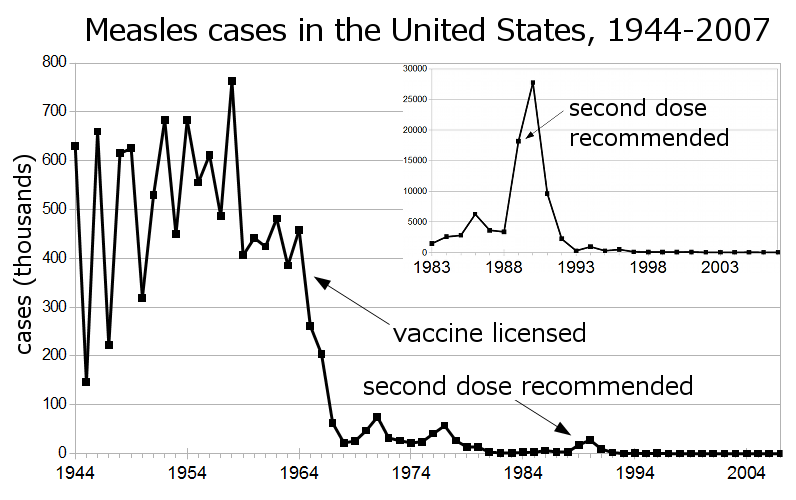
In the 1960s, children throughout America began receiving a vaccination for measles. And as the chart above (via Wikipedia) shows, the vaccine, by and large, made the disease history. But that’s not all that happened. As NPR reported, after widespread use of the vaccine began, “childhood deaths from all infectious diseases plummeted. Even deaths from diseases like pneumonia and diarrhea were cut by half.” Somehow, the measles vaccine was keeping other diseases at bay, too.
And until recently, no one knew why.
The measles vaccine, like most others, is designed to inoculate the patient against a specific disease. The modern measles vaccine (the “MMR”), as the UK’s National Health Service explains, “contains weakened versions of live measles, mumps and rubella viruses. The vaccine works by triggering the immune system to produce antibodies against measles, mumps and rubella.” Those antibodies, though, aren’t useful against other diseases — the MMR shot won’t prevent a child from getting anything else.
But, as noted above, that’s exactly what was happening. Children who were inoculated against the measles were significantly less likely to die from other diseases than children who hadn’t received the vaccine.
At first, the medical community thought this was simply because those receiving vaccinations had better access to medical care than those who didn’t. But when the vaccine made its way to other nations — often poorer nations — the same thing happened: the incidence of measles fell, but so did the incidence of other diseases. So scientists looked for other explanations. And as it turns out, the most likely reason is that measles is more dangerous than we originally thought.
In a paper published in the May 8th issue of Science, a team lead by a Princeton biology postdoc and Emory medical student named Michael Mina explained why: the measles virus didn’t just cause measles, but also weakened the immune system overall. How? As the New York Times reported, “studies suggest that measles infection depletes B and T lymphocytes, specialized white blood cells that produce antibodies that ‘remember’ the measles virus, providing immunity against further attacks.” Mina compared this to amnesia, as he told NPR in the above-linked article:
Well, say you get the chicken pox when you’re 4 years old. Your immune system figures out how to fight it. So you don’t get it again. But if you get measles when you’re 5 years old, it could wipe out the memory of how to beat back the chicken pox.
That’s been known for a while, but the effects were believed to be short-lived, perhaps only as long as the measles virus was active in a person’s system. Mina and team came to a different conclusion. Per their research, this “immune amnesia” can last two or three years — long enough where children are exposed to lots of different diseases to which they have become once again vulnerable.
Avoiding the measles, therefore, also avoids this eradication of the immune system. So while the measles vaccine itself doesn’t increase the body’s ability to fight non-measles disease, the net result is the same: for years after inoculation, the measles shot reduces the spread and effect of other, unrelated childhood diseases.
Bonus Fact: In 2014, per NPR, an estimated 250,000 people contracted measles. 145,000 of them died due to complications from the disease.
From the Archives: The Smallpox Boat: The incredible story of how the smallpox vaccine travelled across the Atlantic.
